Sepsis is the body’s overwhelming and life-threatening response to infection that can lead to tissue damage, organ failure, and death. In other words, it’s your body’s overactive and toxic response to an infection.
It is the third largest cause of death in the UK and kills more people than bowel, breast and prostate cancer combined.
There were over 250,000 cases of sepsis in 2018 according to the UK Sepsis Trust and at least 46,000 people die every year as a result of the condition.
Some people are at higher risk of developing sepsis because they are at higher risk of contracting an infection. These include the very young, the very old, those with chronic illnesses, and those with a weakened or impaired immune system.
But it can affect anyone at any age, even those in good health – and recovery can be a long and difficult journey for those fortunate to survive.
In severe cases of septic shock, the most common cause of death is multi-organ failure due to a loss of blood pressure. To combat this, a range of drugs called vasopressors are administered. These have the effect of constricting the blood vessels in the arms and legs, redirecting the flow to the major organs. Approximately 40% of critical care patients with septicaemia require vasopressor administration. Unfortunately, this necessary regime has serious complications with life changing consequences for many patients.
The primary complication is a condition called disseminated intravascular coagulation (DIC), which occurs when trapped blood in the constricted arteries in the arms and legs, coagulates (or clots) and blocks the vessel. When the drug regime is discontinued and the blood flow returns to the limbs, these clots impair the re-vascularisation and gangrene occurs. Many of these patients then undergo limb salvage and amputation, often in multiple limbs – with mid-calf and above-wrist level amputations not uncommon.
Currently there is no NHS treatment for DIC induced ischaemic and gangrenous limbs other than salvage surgery.
In 1999, Tom and Nicola Ray were newly married and expecting their second child when, almost overnight, their lives were thrown into turmoil. Tom developed sepsis following a dental procedure and within a day of onset, he slipped into a coma. He was 38 years old.
When he woke up five months later, Tom discovered he had undergone quadruple amputations to both hands and feet, with additional facial amputations as a result of sepsis. He couldn’t remember who he was and didn’t recognise his family. During his coma, Nicola gave birth to their second child, but their difficulties were far from over.
Tom and Nicola lost the business they were running together and had to sell their house and move out. There followed several years of reconstructive surgery..
“I had to go through several years of extremely painful facial reconstruction operations to get a cosmetic nose and to make me look not so ugly. But the surgeon at the London Hospital gave up in the end – he is the best in the world but he said there was nothing more they could do about my face. I never understood why but apparently it was too difficult.”
Last year, an extremely moving film detailing Tom’s journey to recovery was released at the Edinburgh Film Festival. It should be seen by everyone.
When Scottish businesswoman Corinne Hutton from Lochwinnoch, fell ill at age 43 in June 2013 after suffering acute pneumonia and sepsis, surgeons were forced to amputate both her hands and her legs below the knee. Prior to her illness, Corinne was a busy small business owner, devoted Mum and regular fitness fanatic, setting herself challenges like running marathons, cycle rides and climbing expeditions to raise money for worthy causes. Earlier this year, Corrine underwent a double hand transplant and is presently recuperating, but like Tom and Nicola, she has since devoted herself to raising awareness of sepsis and its devastating complications and helping those who have lost limbs. Brave and amazing people all.
Five months ago, I wrote about the experience of a friend, Alan Bowell, from Blackpool who contracted sepsis last September and was gravely ill on admission to hospital. Alan had recently started taking medication for Crohn’s Disease – an immunosuppressant called Azathioprine – and was nine days into the course when he became disorientated and shivering uncontrollably.
He wasn’t made aware that immunosuppressant therapy can be a contributory factor in sepsis cases – and consequently, remained ignorant of the clinical signs and symptoms of the disease. Alan thought he was coming down with the flu and didn’t seek any medical help until the following morning when his condition deteriorated significantly. His last memory before he fell unconscious was being helped into the ambulance at home.
Ten days later, when he regained consciousness he discovered gangrene was already established in both feet and the fingers of his right hand and the prognosis was poor. Alan had undergone a colon resection a few days after admission and had a stoma fitted, but a surgeon advised he would require further operations to the gangrenous limbs, before a stoma reversal could be considered.
In cases of vascular insufficiency, with accompanying tissue necrosis and gangrene, a demarcation line is often found encircling the affected limb. This represents the boundary between the truly viable and dead or dying tissue. In limb salvage the level of amputation is determined by the demarcation line to ensure healing takes place.
Three weeks after regaining consciousness, the demarcation line in both Alan’s legs was mid-calf and in his right arm, just above the wrist.
From the previous post you will have read that Alan started a course of hyperbaric oxygen treatment when he was discharged home the following week. I wasn’t aware that he was ill until six weeks after he was admitted – and a month after he regained consciousness. When I visited him on 24 October, I was shocked by his appearance. We’d played guitar together late August and enjoyed a meal and drink. He was in great form.
Within just two months he looked dreadful, lost over two stones and dwarfed in the standard issue NHS high backed chair. It took a bit of time to adjust – just thinking about what he had gone through and what he was now facing. I’m not sure if I was in that position – the very real prospect of losing hands and feet – if I could even face it for a day. But here he was. Knackered, confused, frightened, angry but very determined. At that point, I’m not that sure I understood why.
As he told me what he knew had happened – falling ill, coma, abdominal surgery with bowel resection and stoma – and gangrenous fingers and toes (with established demarcation), I remembered something vaguely similar in the past and mentioned it to Alan.
When the ward doctor called in, we asked him about the possibility of starting hyperbaric oxygen treatment, but he hadn’t heard of it. Nor had any of Alan’s other doctors he was to subsequently see. The vascular and plastic surgeon he was referred to told us there was no evidence that HBOT helped limbs affected by vasopressor administration, but nor did they think it would do any harm.
So, the following week, when he was discharged from hospital, Alan started a seven-day course of HBOT at ‘A Breath for Life’ near Lancaster. After the first one-hour session, he reported feeling ‘tingling and pins and needles’ in both feet and his right hand. By the end of the course the demarcation lines in all three limbs had disappeared and pulses were present again in both feet.
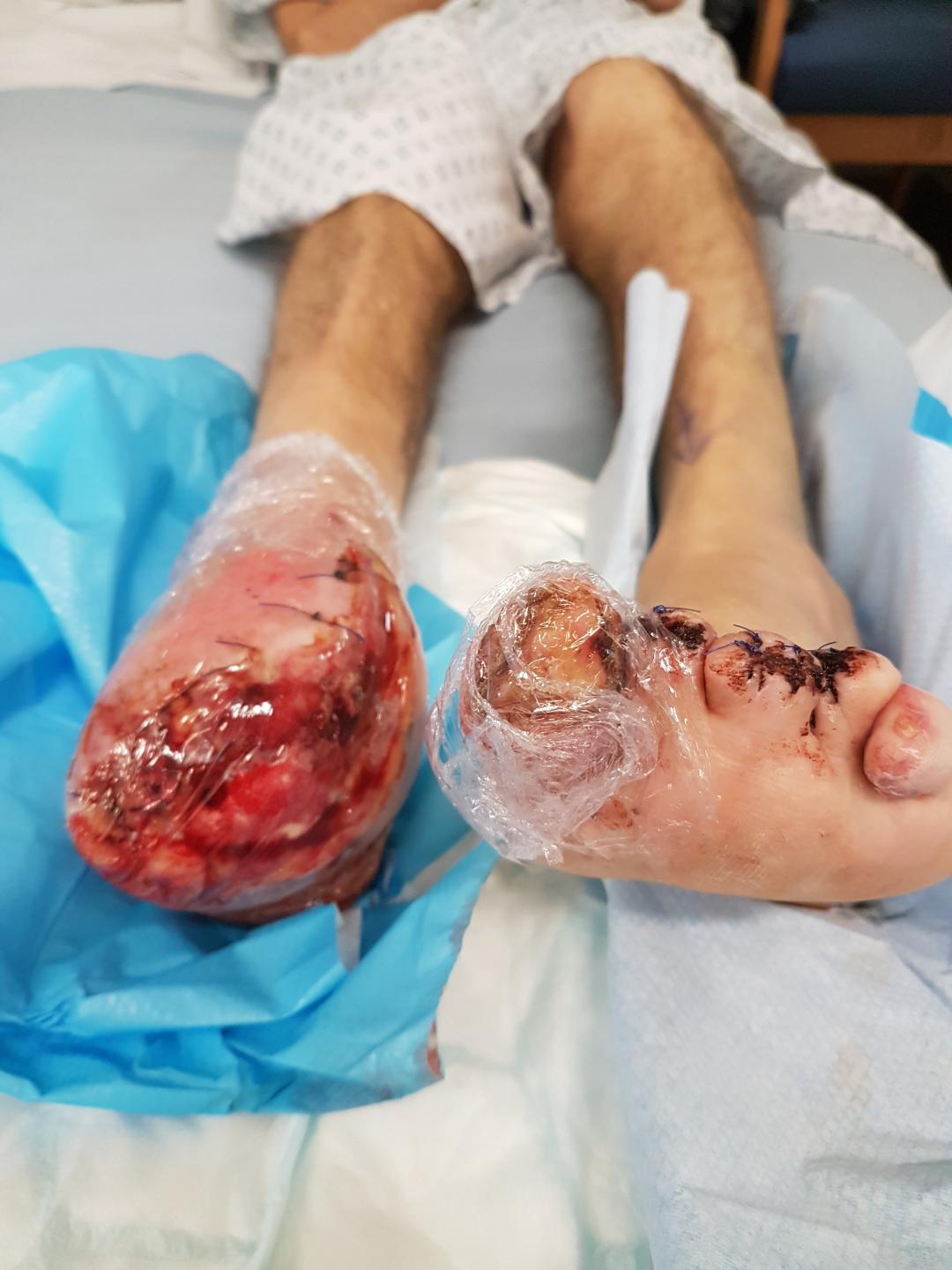
Over the following three months, some recovery of necrotic and gangrenous tissue was established and new skin has since formed. Alan finally underwent salvage surgery in March this year to remove the putrefied tissue of his right forefoot, the apex of three toes on the left – and the tips of two fingers on his right hand.
He is making a good recovery and is hoping the stoma reversal will be scheduled in the very near future. Two weeks ago, he played his first gig since last August and it was a privilege to watch him perform.
I’m not a sepsis or vascular specialist, simply a podiatrist that recalled a similar case a few decades ago and assumed – wrongly, as it turned out – that pressurised oxygen treatment was already playing an important role to play in restoring circulation to limbs affected by vasopressor administration in sepsis management.
To discover that this is not the case in the NHS was astonishing. It certainly worked with Alan, which we are all grateful for – although I can’t help wonder how much more of his limbs could have been saved had the HBOT been started much earlier. Time is the critical factor – once the tissues and blood vessels degrade past a certain point, they are unrecoverable.
But when one considers just how many other patients are facing a similar prospect and prognosis currently, it seems inconceivable that they should be left with no other option than the surgeon’s knife.
Until very recently, I had no idea how HBOT worked in these cases. When I searched for articles online, I discovered no published articles reporting or supporting its use in preventing limb loss in sepsis recovery patients.
However, there were numerous articles on limb loss from vasopressor induced ischaemia following septic shock – and these explain the mechanisms that cause the loss of blood supply and tissue necrosis. The blockage of arteries by clots of coagulated blood – DIC – resonated with me when I read the first article. It is the same mechanism of injury that occurs in severe frostbite – and I’ve known a few people over the years climbers and patients that have lost fingers, toes and limbs from prolonged exposure to the cold.
When searching for DIC in frostbite gangrene – I found several prominent articles citing the use of HBOT for the treatment of frostbite, which explained in detail how pressurised oxygen helped re- vascularise limbs affected by cold induced DIC – even with established high level demarcation and gangrene.
It appears that the mechanism of injury – the coagulated clots in the blood vessels that impair the return of the blood flow – and subsequent tissue death – are the same in severe frostbite and those recovering sepsis patients. In the former, it is extreme cold that closes down the circulation – in the latter it is the drugs used to combat the loss of BP and multi-organ failure in severe septic shock management.
Subsequent searches on different medical and scientific databases have revealed numerous articles citing the use of HBOT for frostbite – many as the ‘gold standard’. Pressure chambers are now installed in most scientific stations in the Artic and Antarctic – as well as various sites in the Himalaya – specifically for that purpose.
Scientists and medics from Norway, Denmark, Russia and Canada use the HBOT chambers in the Artic – and all reports/papers demonstrate favourable outcomes and a considerable reduction in limb/tissue loss.
Recent papers cite a combined regime of HBOT, thrombolytics and manual physiotherapy/massage initiated as soon as possible following injury provide the best outcomes. If this works for frostbite, it may prove beneficial in sepsis care to prevent limb loss.
As Alan remarked, “It seemed like a good positive thing – and what did I have to lose, except the obvious?”
So, although I am no longer in practice, I thought it might be a good idea to report it to someone, especially as it seemed no-one in the NHS had even heard of HBOT, never mind its use for these patients. In January, I wrote to my MP and asked him to notify somebody in the Department of Health and two months later they replied saying following a recent review, HBOT was only now commissioned for decompression sickness in diving injuries and before they’d consider it further, they’d need a detailed proposal from a relevant specialist.
There are no HBOT facilities in the NHS and most of the private/charitable centres use multi-person chambers we are all familiar with. However, single use units for intensive care are used in many other countries. They are inexpensive and simple to operate and take up no more space than a hospital bed.
I’ve since written 98 emails to various people I think might be vaguely interested – the editors and presenters of news programs every time sepsis is mentioned, which is fairly regular these days. Same with newspaper health and medical correspondents who write regularly about tragic cases like Tom and Corinne – and other sepsis patients. To Ministers, shadow Ministers and other politicians – and even places like the Sepsis Trust and other charities.
Unfortunately, I have yet to receive an acknowledgement never mind a response from any one. You’d think I would know better by now….
I’m publishing this now in the hope it gets shared through social media, text or word of mouth – so that those of you who may one day find yourself in a similar predicament and told, like Alan, that nothing that can be done – might now be able to offer a suggestion to the medical team that could be very worthwhile.
You will encounter scepticism if not opposition; the majority of NHS doctors will search internet and find no evidence – and that’s what forms their opinion today – but if you are the victim or relative or friend, please persist and cite this post and the attached articles as evidence.
Hopefully someone else will join up the dots very soon. Of the 200,000 plus survivors of sepsis every year in the UK, a not insignificant number of people will require salvage surgery and amputations as a direct result of the drugs given to save their lives. It really shouldn’t be one or the other.
This may well prove to be a low-cost, simple, safe and evidenced solution for a tragic, horrific condition that the NHS is simply ignoring and leaving to deteriorate without intervention.
Please share if you think it useful or appropriate, thank you.


Great article
Thanks for sharing
https://blogs.mercola.com/sites/vitalvotes/archive/2020/04/05/ny-icu-physician-believes-respirators-may-be-making-covid19-worse.aspx
https://articles.mercola.com/sites/articles/archive/2020/04/05/ozone-therapy.aspx
https://blogs.mercola.com/sites/vitalvotes/archive/2020/04/04/why-molecular-hydrogen-could-prevent-many-covid19-deaths.aspx
vitamin E for gangrene
http://www.doctoryourself.com/estory.htm